Hospital deficits are damaging patient care due to increased wait times, reduced staffing capacity, and a devaluing of healthcare in Ontario, says a new report from the Canadian Centre for Policy Alternatives (CCPA) commissioned by the Ontario Council of Hospital Unions.
“Wait times are a canary in the coal mine,” said Andrew Longhurst, senior researcher and political economist for the CCPA, at a media conference at the Peterborough Public Library on Thursday (May 14).
This new data shows that emergency room and admission wait times at Peterborough Regional Health Centre (PRHC) have both increased significantly over the past five years, with patients waiting up to 110 per cent longer for admission to an inpatient bed.
Report examines deficits at 136 Ontario hospitals
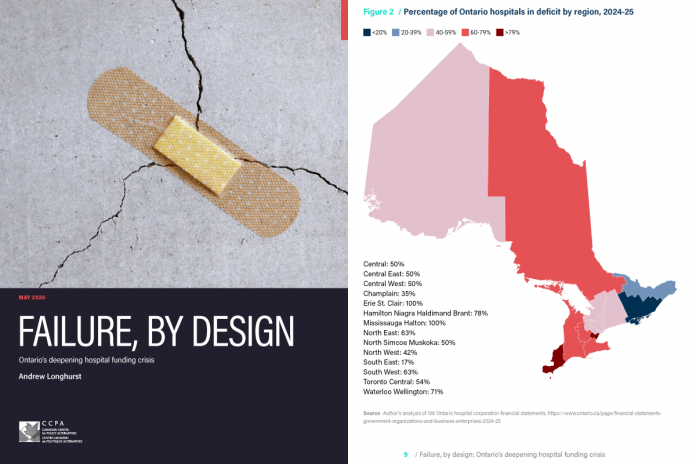
Failure, By Design: Ontario’s deepening hospital funding crisis, written by Longhurst, collates a unique data set of three years of fiscal data from 136 hospitals in Ontario with the intention of understanding the impact of deficits on patient care.
The 26-page report states that “the majority of hospitals had deficits over the last three years,” and said that the most significant expense for hospitals is non-physician staffing compensation. This includes nurses, administrative staff, and other medical professionals.
PRHC saw an operating deficit of $9 million in the 2024/25 fiscal year compared to their annual operating revenue of $448 million, said Longhurst.
Lakeridge Health and Campbellford Memorial Hospital also experienced funding deficits in their most recent fiscal year. The deficits were $20.6 million and $3.2 million respectively.
Longhurst said current projections from the Ontario Hospital Association suggest that 70 per cent or more of hospitals will show a deficit in the current fiscal year.
Michael Hurley, president of the Ontario Council of Hospital Unions (OCHU/CUPE) who joined Longhurst on Thursday, said the report further demonstrates that “the reality is they (hospitals) aren’t funded properly.”
Longhurst’s report breaks down its data analysis by region, demonstrating that hospitals in northern and western communities are disproportionately impacted by deficits. He further said that rural communities such as the Peterborough region are also overrepresented.
The report says that “smaller hospitals made up 61 per cent of the hospitals in deficit but made up only 49 per cent of all Ontario hospitals.” The CCPA defines a small hospital as having an annual operating budget of under $100 million.
One reason given by Longhurst for this disproportionate ratio of smaller hospitals in deficits is because they lack capital reserves and have fewer resources available.
PRHC is part of the 50 per cent of hospitals in the central east region that were in deficit in 2024/25. With an annual operating revenue of $448 million, it is considered one of the larger hospitals that represented “49 per cent of hospitals in deficit and accounted for 51 per cent of Ontario hospitals.”
Increasing ER wait times a sign hospitals are struggling to meet patient demand
A key purpose of the report is to assess how funding deficits impact the quality of care provided to patients.
“Multiple important indicators suggest that hospital funding austerity is undermining care and putting patients at risk,” the report reads.
Longhurst’s report uses emergency department wait times, inpatient wait times, and available staffed beds as measures of the quality and experience of patient care.
“Emergency rooms with long wait times and overcrowding signal that the system is really struggling to meet patient demand,” said Longhurst.
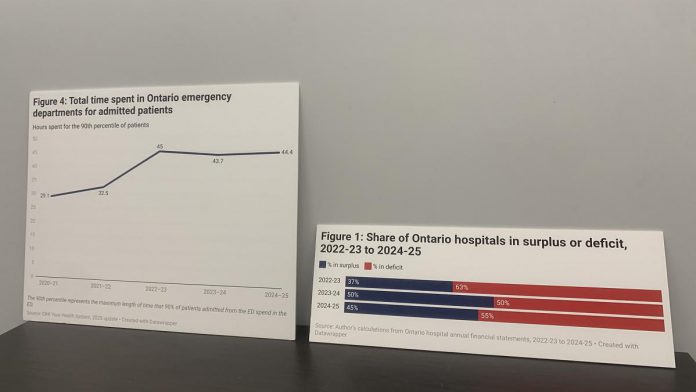
At a provincial level, the report cites data from the Canadian Institute for Health Information which shows the time patients are waiting to receive an initial assessment with a doctor increased by 67 per cent between 2020/21 to 2024/25.
Longhurst said that, at PRHC, initial assessment wait times in the emergency department for the 90th percentile rose from 2.7 hours to 6.1 hours in this same period.
This data places Peterborough as “a bit of an outlier at the high end of the province,” he added.
Hurley explained that, from a frontline perspective, emergency room overcrowding leads to poorer outcomes for patients and indicated concern about the growing prevalence of “hallway medicine.”
Longhurst and Hurley both said that patients being treated in hallways is unacceptable and lacks dignity and respect.
Another factor is the wait times for patients to transition from the emergency department to an inpatient bed and admission to the hospital. According to Longhurst, the wait times for the 90th percentile awaiting admission increased by 52 per cent provincially over a five year period.
At PRHC, 90 per cent of patients must wait 37 hours in the emergency department before they can be admitted for treatment — an increase from 22.7 hours in 2020/21.
Chronic underfunding leads to understaffing and ‘devalues’ contributions of female-led healthcare work to the economy
Inpatient admission is reliant upon available staffed beds, and as such requires the hospital to have adequate staffing levels to provide care to inpatient individuals. The CCPA reports that, in 2022, Ontario had the fewest available beds at 199 per 100,000 people, compared to the Canadian average of 217 beds per 100,000 people.
“There is widespread agreement among analysts that Ontario’s hospital sector is the most undersized in Canada relative to size of the population,” reads the report.
Longhurst highlighted the lack of beds as a factor in increased wait times and overcrowding, saying that per the Financial Accountability Office of Ontario, the number of staffed beds per 100,000 people is projected to decrease from 220 in 2024/25 to 203 in 2027/28.
For his part, Hurley said that there are approximately 200,000 people awaiting surgery, of which 75,000 have been waiting beyond the medically recommended period.
In addition to the report’s analysis of wait times and staffed bed availability, Longhurst looks to factors such as a growing population, inflation, and an aging patient population as reasons for increased costs and demands in the hospital sector.
Both Longhurst and Hurley said that chronic underfunding is an attempt to “devalue” healthcare and the work of hospital staff. The report states that this “devaluing” includes reduced funding for post-secondary education, lowering immigration targets, hospital privatization, and cuts to healthcare service spending.
The CCPA also recognizes the relationship between the devaluation of care work and misogynistic beliefs about women’s contributions to the economy. According to the report, Ontario’s finance minister Peter Bethlenfalvy recently said that “85 per cent of the spending in the budget is actually for social spending (and) about 15 per cent is for infrastructure and the economy.”
“This is a very outdated and sexist belief about what counts as Ontario’s economy,” the report states, defining the “care economy” as including employment in healthcare, social assistance, and educational services. “Work in the care economy is overwhelmingly performed by women in the public sector who pay taxes, support families, and contribute to community wellbeing.”
Hurley expressed similar sentiments, saying the lack of funding for healthcare education and training demonstrates a “bias” towards male-dominated fields such as policing.
Report calls for billions in new hospital funding and workforce strategy and capital plan
Ultimately, the report makes two recommendations to the Ontario government that intend to address chronic underfunding and ensure strong patient care.
The first is to “immediately increase funding” to hospitals to meet both the short-term needs experienced by hospitals with operating deficits and the long-term demands of the patient community.
In March 2026 the Ontario Hospital Association estimated hospitals would need an increase of $2.7 billion in 2025/26 to stabilize service, while the Financial Accountability Office of Ontario estimates $6.4 billion in new spending in for 2026/27 is required to maintain current service levels.
The Ontario government’s 2026/27 budget includes an increase of 3.5 per cent with a further 2.3 per cent increase in 2027/28. Current projections from the Ontario Hospital Association suggest that costs in the hospital sector increase by approximately six per cent annually.
The second recommendation is to “develop a provincial healthcare workforce strategy” to address challenges surrounding recruitment and retention of qualified staff.
The complete report is available at www.policyalternatives.ca.